Writer: Tiffany Whisner, Coles Marketing
 Lose weight. Exercise. Eat healthier. Stay fit. Enjoy life more. Run a marathon. These are some of the most common — and most commonly broken — New Year’s resolutions.
Lose weight. Exercise. Eat healthier. Stay fit. Enjoy life more. Run a marathon. These are some of the most common — and most commonly broken — New Year’s resolutions.
In the U.S., nearly half of people make New Year’s resolutions each year, and many of them revolve around better health. Along with your own health and fitness goals, another part of that plan is to consider the access you have to healthcare facilities and providers in order to make those personal goals more achievable.
Did you ever think about how you get to the gym to do your workout regimen? Or how you get screened with certain equipment for various medical conditions? You may not keep your New Year’s resolution to get fit because you lack the will power or you just don’t feel like working out. But what if there were other barriers beyond your own control?
Meeting the needs of those who need
According to the World Health Organization, more than one billion people, or 15% of the world’s population, have some form of disability. And for a number of reasons, people with disabilities have less access to healthcare services and, therefore, experience unmet healthcare needs.
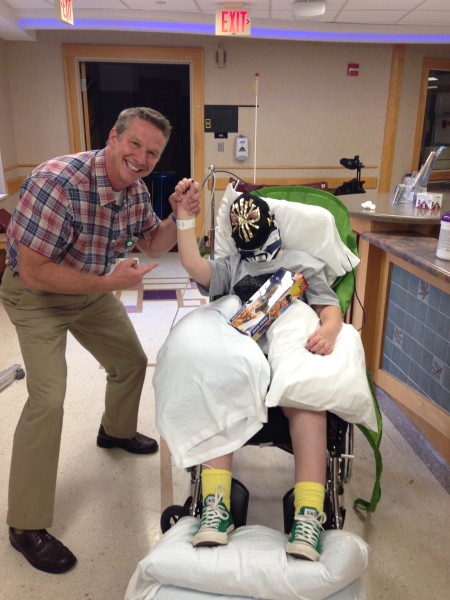 “People with disabilities have access to healthcare, but do they have access to the healthcare they need?” asked Easter Seals Crossroads Medical Director Chuck Dietzen, M.D. “They may have very high needs — including specialists — and you have to factor in the transportation to get to the specialist, how far away they may be and the accessibility of the building. Some of the kids we see at Easter Seals Crossroads are being followed by half a dozen doctors, and orchestrating it all becomes quite an effort.”
“People with disabilities have access to healthcare, but do they have access to the healthcare they need?” asked Easter Seals Crossroads Medical Director Chuck Dietzen, M.D. “They may have very high needs — including specialists — and you have to factor in the transportation to get to the specialist, how far away they may be and the accessibility of the building. Some of the kids we see at Easter Seals Crossroads are being followed by half a dozen doctors, and orchestrating it all becomes quite an effort.”
Dr. Chuck’s career as a pediatric physical medicine and rehabilitation specialist coupled with his commitment to the medically underserved led to his founding of Timmy Global Health in 1997. The organization expands access to healthcare and empowers volunteers to tackle today’s biggest global health challenges.
“In the populations of people with disabilities, they can have extremely complicated medical histories,” Dr. Dietzen said. “It’s an issue throughout their lives, and it’s very difficult transitioning from one doctor to the next as they grow older.” Doctors may be able to identify the healthcare needs of a person with a disability, but can they actually meet the need?
“For example, in Indiana, we only have three pediatric rehab doctors, and in Cincinnati, they have eight or nine,” Dr. Dietzen said. “Is the demand for care in this area going to exceed the supply of doctors to give that care? We manage medications, prescribe therapy, identify durable medical equipment and refer to other doctors. There’s a lot to arrange and coordinate.”
And the red tape and bureaucracy of the healthcare system, especially for people with disabilities, often prevents healthcare needs from being met in a timely and financially-efficient manner.
Getting reimbursed through service
“We need to spend more time with our patients and less time with our documents,” Dr. Dietzen said. “Unfortunately, healthcare these days is often looked at as a business. And the economics of healthcare dictate that unless you really value a certain population, it’s easy to subtly ignore that population. There’s a reason you have women’s and children’s hospitals.”
 Prohibitive costs are just one barrier to healthcare for people with disabilities. Affordability of healthcare and transportation are two main reasons why people with disabilities don’t get the healthcare they need in some low-income countries, according to the World Health Organization. Thirty-two to 33 percent of non-disabled people are unable to afford healthcare compared to 51-53 percent of people with disabilities.
Prohibitive costs are just one barrier to healthcare for people with disabilities. Affordability of healthcare and transportation are two main reasons why people with disabilities don’t get the healthcare they need in some low-income countries, according to the World Health Organization. Thirty-two to 33 percent of non-disabled people are unable to afford healthcare compared to 51-53 percent of people with disabilities.
“For kids with disabilities especially, they are always growing and always going to need a new piece of equipment,” Dr. Dietzen said. “If you have a disability, you can end up in the poor house. With new equipment, making sure you have accessible transportation in addition to seeing doctors, therapists, and specialists, it can really be a challenge to get your healthcare needs taken care of. Third-party payors need to get on board with these issues and help try to solve them.”
Making sure people continue and enhance their independence and avoid having to enter institutional care is the reason behind The Older Blind and Visually Impaired Program, called Chapter 2, a free program to assist senior citizens who are blind or visually impaired at the Wabash Independent Living and Learning (WILL) Center, Inc.
Eliminating the cost barrier for this population of people with visual impairments who are at least age 55, the WILL Center provides low-vision support groups, orientation and mobility training, assistive products and resource referral at no cost to its consumers.
And Danny Wayne Beemer is the “poster child” for helping with that particular community of people.
Beemer has had just slightly more than light perception since birth. He started working for the WILL Center in 2000 and then began to promote The Older Blind and Visually Impaired Program in 2002.
“Working with the WILL Center has really given me a platform to help others, and that means so much to me to be able to do that,” Beemer said. “Through this program, we assess what a person’s challenges are and develop a plan for him or her stay independent as long as possible.”
Beemer leads a team with two other staff members, who are both sighted.
“We cover 13 counties, and we go to each individual home to review and assess the living situation,” he said. “I need the help of my staff to see things, but the seniors we are visiting trust me even more because I know what they are dealing with, and I live it every day.” Beemer highlights the obstacle of transportation for people with disabilities.
“If I didn’t have a driver or a partner with me, I wouldn’t be able to provide these vision services to others,” he said. “What about the transportation challenges for someone who is visually impaired? Especially those in underserved or rural areas. How do they get to the healthcare facility or hospital they have to get to? They rely on someone else. That’s time, effort, and often money, that someone without a disability may take for granted.”
A personal education in care
People with disabilities were more than twice as likely to report finding healthcare provider skills inadequate to meet their needs, four times more likely to report being treated badly, and nearly three times more likely to report being denied care, according to the World Health Organization.
These staggering statistics reflect a lack of knowledge and awareness in the healthcare community.
 “Doctors absolutely need to be more aware of how to treat people with disabilities,” Dr. Dietzen said. “Many questions may go unanswered, and you need to speak to them on a personal level.”
“Doctors absolutely need to be more aware of how to treat people with disabilities,” Dr. Dietzen said. “Many questions may go unanswered, and you need to speak to them on a personal level.”
“Many doctors talk to the other person in the room and not the person with the disability,” Beemer added. “Some won’t talk to you as an individual or address you as the decision maker of your own care. Like when I would go to the eye doctor, they would want to take my hand, as if I hadn’t made my way to their office without having someone with me.”
And for Dr. Dietzen, he also makes sure each pediatric patient is in on his or her own healthcare.
“I have always said to doctors I have trained to talk to the pediatric patient and not just the parents. I know that probably sounds crazy to some, but I always address the child. And they notice that. The same information should be dispensed to the individual with the disability as one without, and it should be said in simple language so they understand but doesn’t make them feel unintelligent,” Dr. Dietzen said.
Just because someone has a physical disability does not mean they have a learning disability.
 “We often make assumptions based on one’s physical appearance, like being in a wheelchair,” Dr. Dietzen said. “People assume that a person with physical deficits may well have cognitive deficits, and that is certainly not always the case.”
“We often make assumptions based on one’s physical appearance, like being in a wheelchair,” Dr. Dietzen said. “People assume that a person with physical deficits may well have cognitive deficits, and that is certainly not always the case.”
Easter Seals Crossroads provides services tailored to meet the specific needs of the individuals served — an individual plan for the individual person.
“When working with people, I want them to learn about their bodies,” Dr. Dietzen said. “The body is something that needs to be taken care of, so I use my hands instead of a reflex hammer. I put the stethoscope in their ears. They need to learn what their body is all about. You find out more in an interactive exam instead of forcing people to do the certain movements you want them to do.”
People with disabilities may have a more difficult journey learning about their bodies because there are less health promotion and prevention activities that target them.
According to the World Health Organization, women with disabilities receive less screening for breast and cervical cancer than women without disabilities. People with intellectual impairments and diabetes are less likely to have their weight checked. And adolescents and adults with disabilities are more likely to be excluded from sex education program.
Health education for people with disabilities also comes in the form of learning about the assistive devices you may use to help your body.
And when working with consumers, Beemer not only assesses what device the person with visual impairments will need, but also works with them to train on that device and know how to use it themselves.
“We have a partnership with Easter Seals Crossroads and INDATA that includes visiting and training blind or visually-impaired seniors with certain assistive technology (AT) devices,” he said. “Along with getting the AT device for each person to use, a trainer will work with the individual and tailor a specific skill set for how to work with that device.”
It’s a look at the person as an individual, a focus on the patient.
The mission of healthcare
“We need to focus on what it is that would heal — not cure — the patient,” Dr. Dietzen said. “I’ve always felt when working with children with disabilities that they need that super normal experience that makes them feel like there’s something exciting ahead. So I always ask my patients: what is a dream of yours you can’t imagine getting to do? It’s a way to keep them looking forward.”

Doctors are spending less time with patients in general, but people with disabilities are particularly vulnerable to deficiencies in healthcare services as well as an inaccessibility to medical equipment and healthcare facilities.
“We need a total revamp of the healthcare system,” Dr. Dietzen said. “We need to dig our heels in and get back to what it’s really about. One of the things to being a great doctor is you need to know what you know and what you don’t. You need to be honest and interactive with the patient, and especially for those with disabilities, you need to talk to them as a person and not talk ‘at’ them.”
“There is hope for the future of healthcare for people with disabilities,” Beemer said. “Better training and better awareness is needed, but it will come. There are some exciting technologies on the horizon to help make things more accessible for people with disabilities and hopefully help them enjoy the things that bring them joy in life.”
“We need to be present and compassionate,” Dr. Dietzen said. “And for everyone, medicine needs to be a mission, not a business.”
